Last updated:
Heel pain is a very common foot problem. The sufferer usually feels pain either under the heel (planter fasciitis) or just behind it (Achilles tendinitis), where the Achilles tendon connects to the heel bone.
Even though heel pain can be severe and sometimes disabling, it is rarely a health threat. Heel pain is typically mild and usually disappears on its own; however, in some cases the pain may persist and become chronic (long-term).
There are 26 bones in the human foot, of which the heel (calcaneus) is the largest. The human heel is designed to provide a rigid support for the weight of the body. When we are walking or running it absorbs the impact of the foot when it hits the ground, and springs us forward into our next stride. Experts say that the stress placed on a foot when walking may be 1.25 times our body weight, and 2.75 times when running. Consequently, the heel is vulnerable to damage, and ultimately pain.
In the majority of cases, heel pain has a mechanical cause. It may also be caused by arthritis, infection, an autoimmune problem trauma, a neurological problem, or some other systemic condition (condition that affects the whole body).
Fast facts on heel pain
Here are some key points about heel pain. More detail and supporting information is in the main article.
- Heel pain is usually felt either under the heel or just behind it.
- Heel pain has a prevalence of 3.6%.
- US studies estimate that 7% of older adults report tenderness under the heel.
- Plantar fasciitis is estimated to account for 8% of all running-related injuries.
- There are 26 bones in the human foot, of which the heel is the largest.
- Pain typically comes on gradually, with no injury to the affected area. It is often triggered by wearing a flat shoe.
- In most cases the pain is under the foot, towards the front of the heel.
- The majority of patients recover with conservative treatments within months.
- Home care such as rest, ice, proper-fitting footwear and foot supports are often enough to ease heel pain.
- To prevent heel pain, it's recommended to reduce the stress on that part of the body.
What are the signs and symptoms of heel pain?
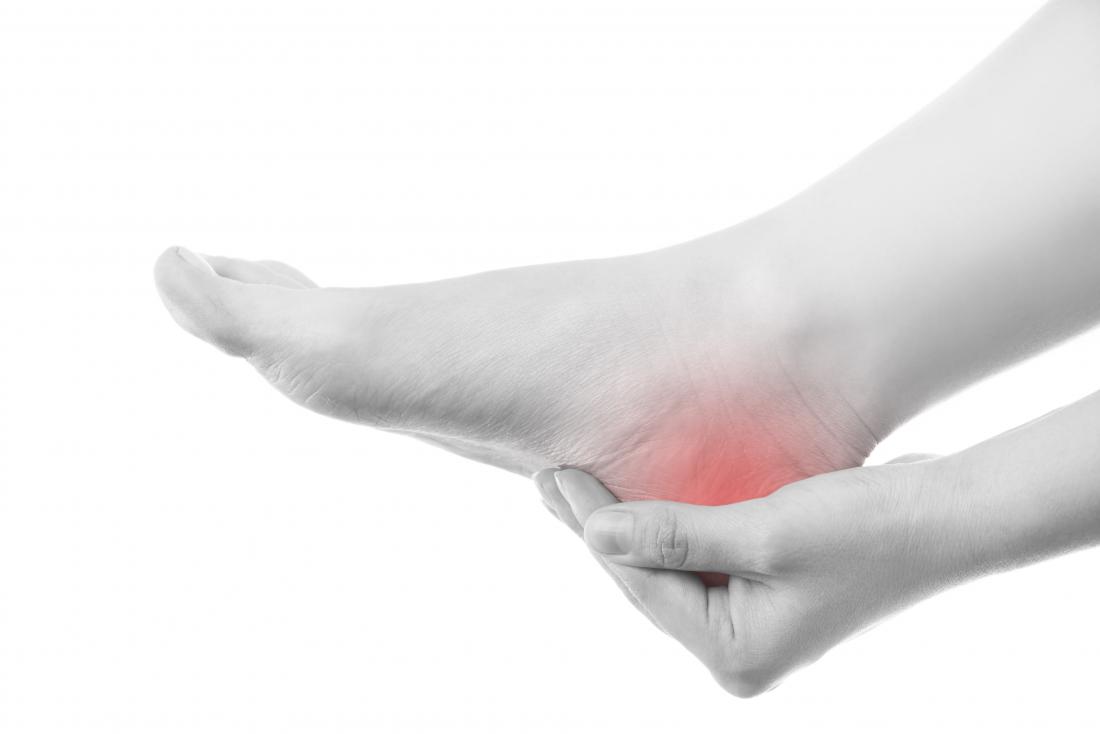
The sufferer usually feels pain either under the heel (planter fasciitis) or just behind it (Achilles tendinitis), where the Achilles tendon connects to the heel bone.
Pain typically comes on gradually, with no injury to the affected area. It is frequently triggered by wearing a flat shoe, such as flip-flop sandals. Flat footwear may stretch the plantar fascia to such an extent that the area becomes swollen (inflamed).
In most cases, the pain is under the foot, toward the front of the heel.
Post-static dyskinesia (pain after rest) - symptoms tend to be worse just after getting out of bed in the morning, and after a period of rest during the day.
After a bit of activity symptoms often improve a bit. However, they may worsen again toward the end of the day.
What are the causes of heel pain?
Heel pain is not usually caused by a single injury, such as a twist or fall, but rather the result of repetitive stress and pounding of the heel.
The most common causes of heel pain are:
- Plantar fasciitis (plantar fasciosis) - inflammation of the plantar fascia. The plantar fascia is a strong bowstring-like ligament that runs from the calcaneum (heel bone) to the tip of the foot. When the plantar fasciitis is stretched too far its soft tissue fibers become inflamed, usually where it attaches to the heel bone. Sometimes the problem may occur in the middle of the foot. The patient experiences pain under the foot, especially after long periods of rest. Some patients have calf-muscle cramps if the Achilles tendon tightens too
- Heel bursitis - inflammation of the back of the heel, the bursa (a fibrous sac full of fluid). Can be caused by landing awkwardly or hard on the heels. Can also be caused by pressure from footwear. Pain is typically felt either deep inside the heel or at the back of the heel. Sometimes the Achilles tendon may swell. As the day progresses the pain usually gets worse
- Heel bumps (pump bumps) - common in teenagers. The heel bone is not yet fully mature and rubs excessively, resulting in the formation of too much bone. Often caused by having a flat foot. Among females can be caused by starting to wear high heels before the bone is fully mature
- Tarsal tunnel syndrome - a large nerve in the back of the foot becomes pinched, or entrapped (compressed). This is a type of compression neuropathy that can occur either in the ankle or foot
- Chronic inflammation of the heel pad - caused either by the heel pad becoming too thin, or heavy footsteps
- Stress fracture - this is a fracture caused by repetitive stress, commonly caused by strenuous exercise, sports or heavy manual work. Runners are particularly prone to stress fracture in the metatarsal bones of the foot. Can also be caused by osteoporosis
- Severs disease (calcaneal apophysitis) - the most common cause of heel pain in child/teenage athletes, caused by overuse and repetitive microtrauma of the growth plates of the calcaneus (heel bone). Children aged from 7-15 are most commonly affected
- Achilles tendonosis (degenerative tendinopathy) - also referred to as tendonitis, tendinosis and tendinopathy. A chronic (long-term) condition associated with the progressive degeneration of the Achilles tendon. Sometimes the Achilles tendon does not function properly because of multiple, minor microscopic tears of the tendon, which cannot heal and repair itself correctly - the Achilles tendon receives more tension than it can cope with and microscopic tears develop. Eventually, the tendon thickens, weakens and becomes painful.
Heel pain may also be caused by:
- Achilles tendon rupture - the tendon of the heel cord behind the ankle is torn
- Bone bruise
- Bone cyst - a solitary fluid-filled cyst (cavity) in a bone
- Gout - levels of uric acid in the blood rise until the level becomes excessive (hyperuricemia), causing urate crystals to build up around the joints. This causes inflammation and severe pain when a gout attack happens
- Neuroma (Morton's neuroma) - a swollen nerve in the ball of the foot, commonly between the base of the second and third toes
- Osteomyelitis - osteomyelitis means infection of the bone or bone marrow; inflammation of the bone due to infection. Osteomyelitis sometimes occurs as a complication of injury or surgery. In some cases, the infection may get into bone tissue from the bloodstream. Patients with osteomyelitis typically experience deep pain and muscle spasms in the inflammation area, as well as fever
- Peripheral neuropathy - neuropathy is a collection of disorders that occurs when nerves of the peripheral nervous system (the part of the nervous system outside of the brain and spinal cord) are damaged. The condition is generally referred to as peripheral neuropathy, and it is most commonly due to damage to nerve axons. Neuropathy usually causes pain and numbness in the hands and feet. It can result from traumatic injuries, infections, metabolic disorders and exposure to toxins. One of the most common causes of neuropathy is diabetes
- Problems with your gait - wrong posture when walking/running
- Rheumatoid arthritis - rheumatoid arthritis, sometimes referred to as rheumatoid disease, is a chronic (long lasting), progressive and disabling auto-immune disease condition that causes inflammation and pain in the joints, the tissue around the joints, and other organs in the human body. Rheumatoid arthritis usually affects the joints in the hands and feet first, but any joint may become affected. Patients with rheumatoid arthritis commonly have stiff joints and feel generally unwell and tired.
When to call a doctor about heel pain
See your doctor as soon as possible if you experience:
- Severe pain accompanied by swelling near your heel
- There is numbness or tingling in the heel, as well as pain and fever
- There is pain in your heel as well as fever
- You are unable to walk normally
- You cannot bend your foot downwards
- You cannot stand with the backs of the feet raised (you cannot rise onto your toes).
You should arrange to see a doctor if:
- The heel pain has persisted for more than one week
- There is still heel pain when you are not standing or walking.
Diagnosing heel pain
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis.
Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
What are the treatment options for heel pain?
Treatment for plantar fasciitis - the vast majority of patients recover with conservative treatments (designed to avoid radical medical therapeutic measures or operative procedures) within months.
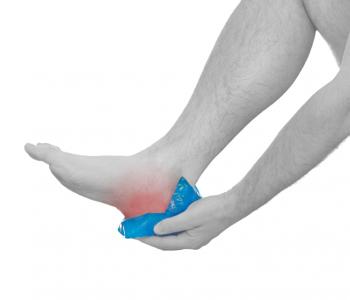
Home care such as rest, ice-pack use, proper-fitting footwear and foot supports are often enough to ease heel pain.
- Non-steroidal anti-inflammatory drugs (NSAIDs) - medications with analgesic (pain reducing), antipyretic (fever reducing) effects. In higher doses they also have anti-inflammatory effects - they reduce inflammation (swelling). Non-steroidaldistinguishes NSAIDs from other drugs which contain steroids, which are also anti-inflammatory. NSAIDs are non-narcotic (they do not induce stupor). For patients with plantar fasciitis they may help with pain and inflammation
- Corticosteroids - a corticosteroid solution is applied over the affected area on the skin; an electric current is used to help absorption. Alternatively, the doctor may decide to inject the medication. However, multiple injections may result in a weakened plantar fascia, significantly increasing the risk of rupture and shrinkage of the fat pad covering the heel bone. Some doctors may use ultrasound to help them make sure they have injected in the right place Corticosteroids are usually recommended when NSAIDs have not helped
- Physical therapy (UK: physiotherapy) - a qualified/specialized physical therapist (UK: physiotherapist) can teach the patient exercises which stretch the plantar fascia and Achilles tendon, as well as strengthening the lower leg muscles, resulting in better stabilization of the ankle and heel. The patient may also be taught how to apply athletic taping, which gives the bottom of the foot better support
- Night splints - the splint is fitted to the calf and foot; the patient keeps it on during sleep. Overnight the plantar fascia and Achilles tendon are held in a lengthened position; this stretches them
- Orthotics - insoles and orthotics (assistive devices) can be useful to correct foot faults, as well as cushioning and cradling the arch during the healing process
- Extracorporeal shock wave therapy - sound waves are aimed at the affected area to encourage and stimulate healing. This type of therapy is only recommended for chronic (long-term) cases, which have not responded to conservative therapy
- Surgery - the plantar fascia is detached from the heel bone. This procedure is only recommended if nothing else works. There is a risk that the arch of the foot is subsequently weakened.
Treatment for heel bursitis - effective treatment depends on the doctor being able to distinguish heel bursitis as a separate condition to plantar fasciitis. The patient may have to use a cushioning insole or heel cup to limit the movements, which are causing the bursitis. This treatment, along with plenty of rest is usually effective. In severe cases, the patient may require a steroid injection.
Treatment for heel bumps - the inflammation behind the heel may be relieved with ice, compression and a change of footwear. There may also be temporary help with Achilles pads, tortoise and heel grip pads. Sometimes the doctor may administer cortisone injections for pain. In severe cases the bumps may have to be removed surgically.
Home care - in cases that are not severe, home care is probably enough to get rid of heel pain.
- Rest - avoid running or standing for long periods, or walking on hard surfaces. Avoid activities that may stress the heels
- Ice - place an ice-pack on the affected area for about 15 minutes. Do not place bare ice directly onto skin
- Footwear - proper-fitting shoes that provide good support are crucial. Athletes should be particularly fussy about the shoes they use when practicing or competing - sports shoes need to be replaced at specific intervals (ask your trainer)
- Foot supports - wedges and heel cups can help relieve symptoms.
Preventing heel pain
Prevention of heel pain involves reducing the stress on that part of the body. Tips include:
- Barefeet - when on hard ground make sure you are wearing shoes
- Bodyweight - if you are overweight there is more stress on the heels when you walk or run. Try to lose weight
- Footwear - footwear that has material which can absorb some of the stress placed on the heel may help protect it. Examples include heel pads. Make sure your shoes fit properly and do not have worn down heels or soles. If you notice a link between a particular pair of shoes and heel pain, stop wearing them
- Rest - if you are especially susceptible to heel pain, try to spend more time resting and less time on your feet. It is best to discuss this point with a specialized health care professional
- Sports - warm up properly before engaging in activities that may place lots of stress on the heels. Make sure you have proper sports shoes for your task.
Source: http://www.medicalnewstoday.com/


No comments:
Post a Comment