Breast cancer
From Wikipedia, the free encyclopedia
| Breast cancer | |
|---|---|
| Classification and external resources | |
 Mammograms showing a normal breast (left) and a cancerous breast (right). | |
| ICD-10 | C50 |
| ICD-9 | 174-175,V10.3 |
| OMIM | 114480 |
| DiseasesDB | 1598 |
| MedlinePlus | 000913 |
| eMedicine | med/2808 med/3287radio/115 plastic/521 |
| MeSH | D001943 |
Breast cancer is a type of cancer originating from breast tissue, most commonly from the inner lining of milk ducts or the lobules that supply the ducts with milk.[1] Cancers originating from ducts are known as ductal carcinomas, while those originating from lobules are known as lobular carcinomas. Breast cancer occurs in humans and other mammals. While the overwhelming majority of human cases occur in women, male breast cancer can also occur.[2]
The benefit versus harms of breast cancer screening is controversial. The characteristics of the cancer determine the treatment which may include surgery, medications (hormonal therapy and chemotherapy), radiation and/or immunotherapy.[3] Surgical provides the single largest benefit, and to increase the likelihood of cure, several chemotherapy regimens are commonly given in addition. Radiation is used after breast-conserving surgery and substantially improves local relapse rates and in many circumstances also overall survival.[4]
Worldwide, breast cancer accounts for 22.9% of all cancers (excluding non-melanoma skin cancers) in women.[5] In 2008, breast cancer caused 458,503 deaths worldwide (13.7% of cancer deaths in women).[5] Breast cancer is more than 100 times more common in women than in men, although men tend to have poorer outcomes due to delays in diagnosis.[6][7]
Prognosis and survival rates for breast cancer vary greatly depending on the cancer type, stage, treatment, and geographical location of the patient. Survival rates in the Western world are high;[6] for example, more than 8 out of 10 women (84%) in England diagnosed with breast cancer survive for at least 5 years.[8] In developing countries, however, survival rates are much poorer.
Signs and symptoms
The first noticeable symptom of breast cancer is typically a lump that feels different from the rest of the breast tissue. More than 80% of breast cancer cases are discovered when the woman feels a lump.[9] The earliest breast cancers are detected by a mammogram.[10]Lumps found in lymph nodes located in the armpits[9] can also indicate breast cancer.
Indications of breast cancer other than a lump may include thickening different from the other breast tissue, one breast becoming larger or lower, a nipple changing position or shape or becoming inverted, skin puckering or dimpling, a rash on or around a nipple, discharge from nipple/s, constant pain in part of the breast or armpit, and swelling beneath the armpit or around the collarbone.[11] Pain ("mastodynia") is an unreliable tool in determining the presence or absence of breast cancer, but may be indicative of other breast healthissues.[9][10][12]
Inflammatory breast cancer is a particular type of breast cancer which can pose a substantial diagnostic challenge. Symptoms may resemble a breast inflammation and may include itching, pain, swelling, nipple inversion, warmth and redness throughout the breast, as well as an orange-peel texture to the skin referred to as peau d'orange;[9] the absence of a discernible lump delays detection dangerously.
Another reported symptom complex of breast cancer is Paget's disease of the breast. This syndrome presents as eczematoid skin changes such as redness and mild flaking of the nipple skin. As Paget's advances, symptoms may include tingling, itching, increased sensitivity, burning, and pain. There may also be discharge from the nipple. Approximately half of women diagnosed with Paget's also have a lump in the breast.[13]
In rare cases, what initially appears as a fibroadenoma (hard movable lump) could in fact be a phyllodes tumor. Phyllodes tumors are formed within the stroma (connective tissue) of the breast and contain glandular as well as stromal tissue. Phyllodes tumors are not staged in the usual sense; they are classified on the basis of their appearance under the microscope as benign, borderline, or malignant.[14]
Occasionally, breast cancer presents as metastatic disease, that is, cancer that has spread beyond the original organ. Metastatic breast cancer will cause symptoms that depend on the location of metastasis. Common sites of metastasis include bone, liver, lung and brain.[15] Unexplained weight loss can occasionally herald an occult breast cancer, as can symptoms of fevers or chills. Bone or joint pains can sometimes be manifestations of metastatic breast cancer, as can jaundice or neurological symptoms. These symptoms are called non-specific, meaning they could be manifestations of many other illnesses.[16]
Most symptoms of breast disorders, including most lumps, do not turn out to represent underlying breast cancer. Less than 20% of lumps for example are cancer[17] and benign breast diseases such as mastitis and fibroadenoma of the breast are more common causes of breast disorder symptoms. Nevertheless, the appearance of a new symptom should be taken seriously by both patients and their doctors, because of the possibility of an underlying breast cancer at almost any age.
Risk factors
Main article: Risk factors of breast cancer
The primary risk factors for breast cancer are female sex and older age.[19] Other potential risk factors include: lack of childbearing or breastfeeding,[20] higher hormone levels,[21][22]diet and obesity.
[edit]Lifestyle
See also: List of breast carcinogenic substances
Smoking tobacco appears to increase the risk of breast cancer with the greater the amount of smoked and the earlier in life smoking began the higher the risk.[23] In those who are long term smokers the risk is increased 35% to 50%.[23] A lack of physical activity has been linked to ~10% of cases.[24]
The association between breast feeding and breast cancer has not been clearly determined with some studies finding support for an association and others not.[25] In the 1980s theabortion–breast cancer hypothesis posited that induced abortion increased the risk of developing breast cancer.[26] This hypothesis has been the subject of extensive scientific inquiry which has concluded that neither miscarriages nor abortions are associated.[27] There may be an association between oral contraceptives and the development of premenopausal breast cancer.[28] Whether or not this association is causal is debated and if there is indeed a link the absolute effect is small.[29][30] In those with BRCA1 or BRCA2 mutations or a family history modern OCPs do not appear to affect the subsequent risk of breast cancer.[31][32]
There is a relationship between diet and breast cancer including an increased risk with a high fat diet,[33] alcohol intake,[34] and obesity.[35] Dietary iodine deficiency may also play a role.[36]
Other risk factors include radiation,[37] and shift-work.[38] A number of chemicals have also been linked including: polychlorinated biphenyls, polycyclic aromatic hydrocarbons,organic solvents[39] and a number of pesticides.[40] Although the radiation from mammography is a low dose, it is estimated that yearly screening from 40 to 80 years of age will cause ~225 cases of fatal breast cancer per million women screened.[41]
[edit]Genetics
Some genetic susceptibility may play a minor role in most cases.[42] Overall, however, genetics is believed to be the primary cause of 5–10% of all cases.[43] In those with zero, one or two affected relatives, the risk of breast cancer before the age of 80 is 7.8%, 13.3%, and 21.1% with a subsequent mortality from the disease of 2.3%, 4.2%, and 7.6% respectively.[44] In those with a first degree relative with the disease the risk of breast cancer between the age of 40 and 50 is double that of the general population.[45]
In less than 5% of cases, genetics plays a more significant role by causing a hereditary breast–ovarian cancer syndrome.[42] This includes those who carry the BRCA1 and BRCA2gene mutation.[42] These mutations account for up to 90% of the total genetic influence with a risk of breast cancer of 60–80% in those affected.[43] Other significant mutations include: p53 (Li-Fraumeni syndrome), PTEN (Cowden syndrome), and STK11 (Peutz–Jeghers syndrome), CHEK2, ATM, BRIP1, and PALB2.[43] In 2012, researchers said that there are four genetically distinct types of the breast cancer and that in each type, hallmark genetic changes lead to many cancers.[46]
[edit]Medical conditions
Certain breast changes: atypical hyperplasia and lobular carcinoma in situ found in benign breast conditions such as fibrocystic breast changes are correlated with an increased breast cancer risk.
Pathophysiology
Main article: Carcinogenesis
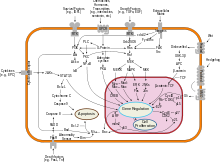
Breast cancer, like other cancers, occurs because of an interaction between an environmental (external) factor and a genetically susceptible host. Normal cells divide as many times as needed and stop. They attach to other cells and stay in place in tissues. Cells become cancerous when they lose their ability to stop dividing, to attach to other cells, to stay where they belong, and to die at the proper time.
Normal cells will commit cell suicide (apoptosis) when they are no longer needed. Until then, they are protected from cell suicide by several protein clusters and pathways. One of the protective pathways is the PI3K/AKT pathway; another is the RAS/MEK/ERK pathway. Sometimes the genes along these protective pathways are mutated in a way that turns them permanently "on", rendering the cell incapable of committing suicide when it is no longer needed. This is one of the steps that causes cancer in combination with other mutations. Normally, the PTEN protein turns off the PI3K/AKT pathway when the cell is ready for cell suicide. In some breast cancers, the gene for the PTEN protein is mutated, so the PI3K/AKT pathway is stuck in the "on" position, and the cancer cell does not commit suicide.[47]
Mutations that can lead to breast cancer have been experimentally linked to estrogen exposure.[48]
Failure of immune surveillance, the removal of malignant cells throughout one's life by the immune system.[49] Abnormal growth factorsignaling in the interaction between stromal cells and epithelial cells can facilitate malignant cell growth.[50][51] In breast adipose tissue, overexpression of leptin leads to increased cell proliferation and cancer.[52]
In the United States, 10 to 20 percent of patients with breast cancer and patients with ovarian cancer have a first- or second-degree relative with one of these diseases. The familial tendency to develop these cancers is called hereditary breast—ovarian cancer syndrome. The best known of these, the BRCA mutations, confer a lifetime risk of breast cancer of between 60 and 85 percent and a lifetime risk of ovarian cancer of between 15 and 40 percent. Some mutations associated with cancer, such as p53, BRCA1 and BRCA2, occur in mechanisms to correct errors in DNA. These mutations are either inherited or acquired after birth. Presumably, they allow further mutations, which allow uncontrolled division, lack of attachment, and metastasis to distant organs.[37][53] However there is strong evidence of residual risk variation that goes well beyond hereditary BRCA gene mutations between carrier families. This is caused by unobserved risk factors.[54] This implicates environmental and other causes as triggers for breast cancers. The inherited mutation in BRCA1 or BRCA2 genes can interfere with repair of DNA cross links and DNA double strand breaks (known functions of the encoded protein)[55] These carcinogens cause DNA damage such as DNA cross links and double strand breaks that often require repairs by pathways containing BRCA1 and BRCA2.[56][57] However, mutations in BRCA genes account for only 2 to 3 percent of all breast cancers.[58] About half of hereditary breast–ovarian cancer syndromes involve unknown genes.
Diagnosis
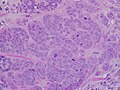
Most types of breast cancer are easy to diagnose by microscopic analysis of the biopsy. There are however, rarer types of breast cancer that require specialized lab exams.
While screening techniques are useful in determining the possibility of cancer, a further testing is necessary to confirm whether a lump detected on screening is cancer, as opposed to a benign alternative such as a simple cyst.
Very often the results of noninvasive examination, mammography and additional tests that are performed in special circumstances such as ultrasound or MR imaging are sufficient to warrant excisional biopsy as the definitive diagnostic and curative method.
Both mammography and clinical breast exam, also used for screening, can indicate an approximate likelihood that a lump is cancer, and may also detect some other lesions.[59]When the tests are inconclusive Fine Needle Aspiration and Cytology (FNAC) may be used which is a confirmatory test. FNAC may be done in a GP's office using local anaesthetic if required, involves attempting to extract a small portion of fluid from the lump. Clear fluid makes the lump highly unlikely to be cancerous, but bloody fluid may be sent off for inspection under a microscope for cancerous cells. Together, these three tools can be used to diagnose breast cancer with a good degree of accuracy.
Other options for biopsy include core biopsy, where a section of the breast lump is removed, and an excisional biopsy, where the entire lump is removed.
In addition vacuum-assisted breast biopsy (VAB) may help diagnose breast cancer among patients with a mammographically detected breast in women.[60]
[edit]Classification
Main article: Breast cancer classification
Breast cancers are classified by several grading systems. Each of these influences the prognosis and can affect treatment response. Description of a breast cancer optimally includes all of these factors.
- Histopathology. Breast cancer is usually classified primarily by its histological appearance. Most breast cancers are derived from the epithelium lining the ducts or lobules, and these cancers are classified as ductal or lobular carcinoma. Carcinoma in situ is growth of low grade cancerous or precancerous cells within a particular tissue compartment such as the mammary duct without invasion of the surrounding tissue. In contrast, invasive carcinoma does not confine itself to the initial tissue compartment.[61]
- Grade. Grading compares the appearance of the breast cancer cells to the appearance of normal breast tissue. Normal cells in an organ like the breast become differentiated, meaning that they take on specific shapes and forms that reflect their function as part of that organ. Cancerous cells lose that differentiation. In cancer, the cells that would normally line up in an orderly way to make up the milk ducts become disorganized. Cell division becomes uncontrolled. Cell nuclei become less uniform. Pathologists describe cells as well differentiated (low grade), moderately differentiated (intermediate grade), and poorly differentiated (high grade) as the cells progressively lose the features seen in normal breast cells. Poorly differentiated cancers (the ones whose tissue is least like normal breast tissue) have a worse prognosis.
- Stage. Breast cancer staging using the TNM system is based on the size of the tumor (T), whether or not the tumor has spread to the lymph nodes (N) in the armpits, and whether the tumor has metastasized (M) (i.e. spread to a more distant part of the body). Larger size, nodal spread, and metastasis have a larger stage number and a worse prognosis.
The main stages are:- Stage 0 is a pre-cancerous or marker condition, either ductal carcinoma in situ (DCIS) or lobular carcinoma in situ (LCIS).
- Stages 1–3 are within the breast or regional lymph nodes.
- Stage 4 is 'metastatic' cancer that has a less favorable prognosis.
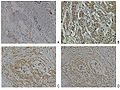
- Receptor status. Breast cancer cells have receptors on their surface and in their cytoplasm and nucleus. Chemical messengers such as hormones bind to receptors, and this causes changes in the cell. Breast cancer cells may or may not have three important receptors: estrogen receptor (ER), progesterone receptor (PR), and HER2.
ER+ cancer cells depend on estrogen for their growth, so they can be treated with drugs to block estrogen effects (e.g. tamoxifen), and generally have a better prognosis. HER2+ breast cancer had a worse prognosis,[62] but HER2+ cancer cells respond to drugs such as the monoclonal antibody trastuzumab (in combination with conventional chemotherapy), and this has improved the prognosis significantly.[63] Cells with none of these receptors are called triple negative although they frequently express receptors for other hormones such as androgen receptor and prolactin receptor.
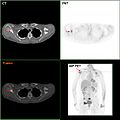
In cases of breast cancer with low risk for metastasis, the risks associated with PET scans, CT scans, or bone scans outweigh the possible benefits.[64][65] This is because these procedures expose the patient to a substantial amount of potentially dangerous ionizing radiation.
- DNA assays. DNA testing of various types including DNA microarrays have compared normal cells to breast cancer cells. The specific changes in a particular breast cancer can be used to classify the cancer in several ways, and may assist in choosing the most effective treatment for that DNA type.
[edit]Prevention
Women may reduce their risk of breast cancer by maintaining a healthy weight, drinking less alcohol, being physically active and breastfeeding their children.[66] These modifications might prevent 38% of breast cancers in the US, 42% in the UK, 28% in Brazil and 20% in China.[66] The benefits with moderate exercise such as brisk walking are seen at all age groups including postmenopausal women.[66][67] Prophylactic bilateral mastectomy may be considered in people with BRCA1 and BRCA2 mutations.[68][69]Tamoxifen and raloxifene are able to reduce the risk of breast cancer but increase the risk of thromboembolism.[70] The benefits of breast cancer reduction continues for at least five years after stoping these medications.[71]
[edit]Screening
Main article: Breast cancer screening
Breast cancer screening refers to testing otherwise-healthy women for breast cancer in an attempt to achieve an earlier diagnosis under the assumption that early detection will improve outcomes. A number of screening test have been employed including: clinical and self breast exams, mammography, genetic screening, ultrasound, and magnetic resonance imaging.
A clinical or self breast exam involves feeling the breast for lumps or other abnormalities. Clinical breast exams are performed by health care providers, while self breast exams are performed by the person themselves.[72] Evidence dose not support the effectiveness of either type of breast exam, as by the time a lump is large enough to be found it is likely to have been growing for several years and thus soon be large enough to be found without an exam.[73][74] Mammographic screening for breast cancer uses X-rays to examine the breast for any uncharacteristic masses or lumps. During a screening, the breast is compressed and a technician takes photos from multiple angles. A general mammogram takes photos of the entire breast, while a diagnostic mammogram focuses on a specific lump or area of concern.[75]
A number of national bodies continue to recommend breast cancer screening. For the average woman, the U.S. Preventive Services Task Force recommends mammography every two years in women between the ages of 50 and 74,[74] the Council of Europe recommends mammography between 50 and 69 with most programs using a 2 year frequency,[76]and in Canada screening is recommended between the ages of 50 and 74 at a frequency of 2 to 3 years.[77] These task force reports point out that in addition to unnecessary surgery and anxiety, the risks of more frequent mammograms include a small but significant increase in breast cancer induced by radiation.[78] Whether MRI as a screening method has greater harms or benefits when compared to standard mammography is not known.[74]
The Cochrane Collaboration (2011) states that the best quality evidence neither demonstrates a reduction in either cancer specific, nor a reduction in all cause mortality from screening mammography.[79] When less rigorous trials are added to the analysis there is a reduction in breast cancer specific mortality of 0.05% (a relative decrease of 15%).[79]Screening results in a 30% increase in rates of over-diagnosis and over-treatment, resulting in the view that it is not clear whether mammography screening does more good or harm.[79] Cochrane states that, due to recent improvements in breast cancer treatment, and the risks of false positives from breast cancer screening leading to unnecessary treatment, "it therefore no longer seems reasonable to attend for breast cancer screening" at any age.[80]
[edit]Management
Main article: Breast cancer management
The management of breast cancer depending on various factors, including the stage of the cancer. Breast cancer is usually treated with surgery and then possibly with chemotherapy or radiation, or both. A multidisciplinary approach is preferable.[81] Hormone positive cancers are treated with long term hormone blocking therapy. Treatments are given with increasing aggressiveness according to the prognosis and risk of recurrence.
[edit]Surgery
Surgery involves the physical removal of the tumor, typically along with some of the surrounding tissue and frequently sentinel lymph node biopsy.
Standard surgeries include:
- Mastectomy: Removal of the whole breast.
- Quadrantectomy: Removal of one quarter of the breast.
- Lumpectomy: Removal of a small part of the breast.
If the patient desires, then breast reconstruction surgery, a type of cosmetic surgery, may be performed to create an aesthetic appearance. In other cases, women use breast prostheses to simulate a breast under clothing, or choose a flat chest. Nipple/areola prostheses can be used at any time following the mastectomy.
[edit]Medication
Drugs used after and in addition to surgery are called adjuvant therapy. Chemotherapy or other types of therapy prior to surgery are called neoadjuvant therapy.
There are currently three main groups of medications used for adjuvant breast cancer treatment: hormone blocking therapy, chemotherapy, and monoclonal antibodies.
- Hormone blocking therapy
- Some breast cancers require estrogen to continue growing. They can be identified by the presence of estrogen receptors (ER+) and progesterone receptors (PR+) on their surface (sometimes referred to together as hormone receptors). These ER+ cancers can be treated with drugs that either block the receptors, e.g. tamoxifen (Nolvadex), or alternatively block the production of estrogen with an aromatase inhibitor, e.g. anastrozole (Arimidex)[82] or letrozole (Femara). Aromatase inhibitors, however, are only suitable for post-menopausal patients. This is because the active aromatase in postmenopausal women is different from the prevalent form in premenopausal women, and therefore these agents are ineffective in inhibiting the predominant aromatase of premenopausal women.[83]
- Chemotherapy
- Predominately used for stage 2–4 disease, being particularly beneficial in estrogen receptor-negative (ER-) disease. They are given in combinations, usually for 3–6 months. One of the most common treatments is cyclophosphamide plus doxorubicin (Adriamycin), known as AC. Most chemotherapy medications work by destroying fast-growing and/or fast-replicating cancer cells either by causing DNA damage upon replication or other mechanisms; these drugs also damage fast-growing normal cells where they cause serious side effects. Damage to the heart muscle is the most dangerous complication of doxorubicin. Sometimes a taxane drug, such as docetaxel, is added, and the regime is then known as CAT; taxane attacks the microtubules in cancer cells. Another common treatment, which produces equivalent results, is cyclophosphamide, methotrexate, and fluorouracil (CMF). (Chemotherapy can literally refer to any drug, but it is usually used to refer to traditional non-hormone treatments for cancer.)[citation needed]
- Monoclonal antibodies
- Trastuzumab (Herceptin), a monoclonal antibody to HER2, has improved the 5-year disease free survival of stage 1–3 HER2+ breast cancers to about 87% (overall survival 95%).[84] Trastuzumab, however, is expensive, and approximately 2% of patients suffer significant heart damage.[85] Other monoclonal antibodies are also undergoing clinical trials. Trastuzumab is only effective in patients with HER2 amplification/overexpression.
Between 25 and thirty percent of breast cancers have an amplification of the HER2 gene or overexpression of its protein product.[86] This receptor is normally stimulated by a growth factor which causes the cell to divide; in the absence of the growth factor, the cell will normally stop growing. Overexpression of this receptor in breast cancer is associated with increased disease recurrence and worse prognosis.
[edit]Radiation
Radiotherapy is given after surgery to the region of the tumor bed and regional lymph nodes, to destroy microscopic tumor cells that may have escaped surgery. It may also have a beneficial effect on tumor microenvironment.[88][89] Radiation therapy can be delivered as external beam radiotherapy or as brachytherapy (internal radiotherapy). Conventionally radiotherapy is given after the operation for breast cancer. Radiation can also be given at the time of operation on the breast cancer- intraoperatively. The largest randomised trial to test this approach was the TAR-GIT-A Trial[90] which found that targeted intraoperative radiotherapy was equally effective at 4-years as the usual several weeks' of whole breast external beam radiotherapy.[91] Radiation can reduce the risk of recurrence by 50–66% (1/2 – 2/3 reduction of risk) when delivered in the correct dose[92] and is considered essential when breast cancer is treated by removing only the lump (Lumpectomy or Wide local excision).
[edit]Prognosis
A prognosis is a prediction of outcome and the probability of progression-free survival (PFS) or disease-free survival (DFS). These predictions are based on experience with breast cancer patients with similar classification. A prognosis is an estimate, as patients with the same classification will survive a different amount of time, and classifications are not always precise. Survival is usually calculated as an average number of months (or years) that 50% of patients survive, or the percentage of patients that are alive after 1, 5, 15, and 20 years. Prognosis is important for treatment decisions because patients with a good prognosis are usually offered less invasive treatments, such as lumpectomy and radiation or hormone therapy, while patients with poor prognosis are usually offered more aggressive treatment, such as more extensive mastectomy and one or more chemotherapy drugs.
Prognostic factors are reflected in the classification scheme for breast cancer including stage, (i.e., tumor size, location, whether disease has spread to lymph nodes and other parts of the body), grade, recurrence of the disease, and the age and health of the patient. The Nottingham Prognostic Index is a commonly used prognostic tool.
The stage of the breast cancer is the most important component of traditional classification methods of breast cancer, because it has a greater effect on the prognosis than the other considerations. Staging takes into consideration size, local involvement, lymph node status and whether metastatic disease is present. The higher the stage at diagnosis, the poorer the prognosis. The stage is raised by the invasiveness of disease to lymph nodes, chest wall, skin or beyond, and the aggressiveness of the cancer cells. The stage is lowered by the presence of cancer-free zones and close-to-normal cell behaviour (grading). Size is not a factor in staging unless the cancer is invasive. For example, Ductal Carcinoma In Situ (DCIS) involving the entire breast will still be stage zero and consequently an excellent prognosis with a 10yr disease free survival of about 98%.[93]
The breast cancer grade is assessed by comparison of the breast cancer cells to normal breast cells. The closer to normal the cancer cells are, the slower their growth and the better the prognosis. If cells are not well differentiated, they will appear immature, will divide more rapidly, and will tend to spread. Well differentiated is given a grade of 1, moderate is grade 2, while poor or undifferentiated is given a higher grade of 3 or 4 (depending upon the scale used). The most widely used grading system is the Nottingham scheme;[94]details are provided in the discussion of breast cancer grade.
The presence of estrogen and progesterone receptors in the cancer cell is important in guiding treatment. Those who do not test positive for these specific receptors will not be able to respond to hormone therapy, and this can affect their chance of survival depending upon what treatment options remain, the exact type of the cancer, and how advanced the disease is.
In addition to hormone receptors, there are other cell surface proteins that may affect prognosis and treatment. HER2 status directs the course of treatment. Patients whose cancer cells are positive for HER2 have more aggressive disease and may be treated with the 'targeted therapy', trastuzumab (Herceptin), a monoclonal antibody that targets this protein and improves the prognosis significantly.
Younger women tend to have a poorer prognosis than post-menopausal women due to several factors. Their breasts are active with their cycles, they may be nursing infants, and may be unaware of changes in their breasts. Therefore, younger women are usually at a more advanced stage when diagnosed. There may also be biologic factors contributing to a higher risk of disease recurrence for younger women with breast cancer.[95]
High mammographic breast density, which is a marker of increased risk of developing breast cancer, may not mean an increased risk of death among breast cancer patients, according to a 2012 report of a study involving 9232 women by the National Cancer Institute (NCI).[96]
Since breast cancer in males is usually detected at later stages outcome are typically worse.[97]
[edit]Psychological aspects
The emotional impact of cancer diagnosis, symptoms, treatment, and related issues can be severe. Most larger hospitals are associated with cancer support groups which provide a supportive environment to help patients cope and gain perspective from cancer survivors. Online cancer support groups are also very beneficial to cancer patients, especially in dealing with uncertainty and body-image problems inherent in cancer treatment.
Not all breast cancer patients experience their illness in the same manner. Factors such as age can have a significant impact on the way a patient copes with a breast cancer diagnosis. Premenopausal women with estrogen-receptor positive breast cancer must confront the issues of early menopause induced by many of the chemotherapy regimens used to treat their breast cancer, especially those that use hormones to counteract ovarian function.[98]
On the other hand, a small 2007 study conducted by researchers at the College of Public Health of the University of Georgia suggested a need for greater attention to promoting functioning and psychological well-being among older cancer survivors, even when they may not have obvious cancer-related medical complications.[99] The study found that older breast cancer survivors showed multiple indications of decrements in their health-related quality of life, and lower psychosocial well-being than a comparison group. Survivors reported no more depressive symptoms or anxious mood than the comparison group, however, they did score lower in measures of positive psychosocial well-being, and reported more depressed mood and days affected by fatigue. As the incidence of breast cancer in women over 50 rises and survival rates increase, breast cancer is increasingly becoming a geriatric issue that warrants both further research and the expansion of specialized cancer support services tailored for specific age groups.[99]
[edit]Prognostic tool
The NPI Nottingham Prognostic Index is a useful tool in assessing the prognosis
- Stage 1 cancers (and DCIS) have an excellent prognosis and are generally treated with lumpectomy and sometimes radiation.[100] HER2+ cancers should be treated with thetrastuzumab(Herceptin) regime.[101] Chemotherapy is uncommon for other types of stage 1 cancers.
- Stage 2 and 3 cancers with a progressively poorer prognosis and greater risk of recurrence are generally treated with surgery (lumpectomy or mastectomy with or without lymph node removal), chemotherapy (plus trastuzumab for HER2+ cancers) and sometimes radiation (particularly following large cancers, multiple positive nodes or lumpectomy).
- Stage 4, metastatic cancer, (i.e. spread to distant sites) has poor prognosis and is managed by various combination of all treatments from surgery, radiation, chemotherapy and targeted therapies. 10-year survival rate is 5% without treatment and 10% with optimal treatment.[102]
[edit]Epidemiology
Main article: Epidemiology of breast cancer
Worldwide, breast cancer is the most common invasive cancer in women. (The most common form of cancer is non-invasive non-melanoma skin cancer; non-invasive cancers are generally easily cured, cause very few deaths, and are routinely excluded from cancer statistics.) Breast cancer comprises 22.9% of invasive cancers in women[5] and 16% of all female cancers.[104]
In 2008, breast cancer caused 458,503 deaths worldwide (13.7% of cancer deaths in women and 6.0% of all cancer deaths for men and women together).[5] Lung cancer, the second most common cause of cancer-related death in women, caused 12.8% of cancer deaths in women (18.2% of all cancer deaths for men and women together).[5]
The incidence of breast cancer varies greatly around the world: it is lowest in less-developed countries and greatest in the more-developed countries. In the twelve world regions, the annual age-standardized incidence rates per 100,000 women are as follows: in Eastern Asia, 18; South Central Asia, 22; sub-Saharan Africa, 22; South-Eastern Asia, 26; North Africa and Western Asia, 28; South and Central America, 42; Eastern Europe, 49; Southern Europe, 56; Northern Europe, 73; Oceania, 74; Western Europe, 78; and in North America, 90.[105]
The number of cases worldwide has significantly increased since the 1970s, a phenomenon partly attributed to the modern lifestyles.[106][107] Breast cancer is strongly related to age with only 5% of all breast cancers occurring in women under 40 years old.

.jpg)